Skeletal Muscle Metastases Arising from Renal Cell Carcinoma in a 58-Year-Old Male: A Case Report
Original Article | Volume 6 | Issue 3 | JBST September – December 2020 | Page 20-25 | Sybill Sue M. Moser, Edwin Joseph R. Guerzon, John Christopher R. Ragasa DOI: 10.13107/jbst.2020.v06i03.035
Author: Sybill Sue M. Moser[1], Edwin Joseph R. Guerzon[1], John Christopher R. Ragasa[1]
[1]Department of Orthopedics, Institute of Orthopedics and Sports Medicine, St. Luke’s Medical Center – Quezon City, Manila, Philippines.
Address of Correspondence:
Dr. Sybill Sue M. Moser
2632 Molave St. United Hills Village,
Parañaque City, Metro Manila, Philippines.
E-mail: sybillsuemoser@gmail.com
Introduction: Renal cell carcinoma (RCC) is the most common malignant kidney tumor, commonly metastasizing to the lung, lymph nodes, bones, and brain. Here, we present a rare case of renal cell skeletal muscle metastases (SMMs), accounting for only <1% of all RCC metastases.
Methods: This is a descriptive report on the clinical course, diagnostic investigations, and surgical treatment of a case of SMM in a patient previously diagnosed with RCC.
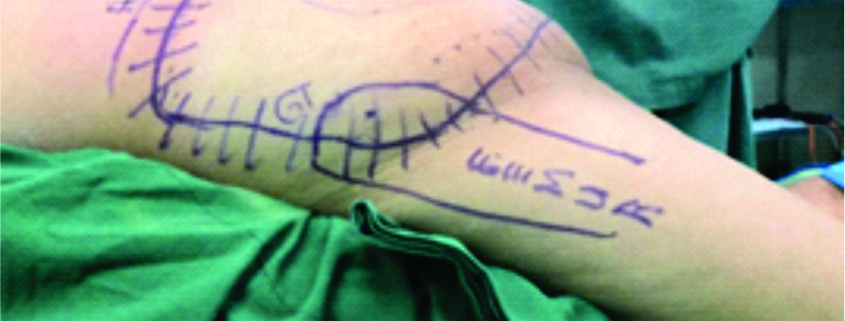
Results: This is a 58-year-old male who previously underwent radical nephrectomy for RCC, presenting with a 5-month history of a rapidly enlarging left gluteal mass. The mass was confirmed to be renal clear cell metastasis through percutaneous biopsy. On magnetic resonance imaging, two heterogeneously enhancing lesions in the left gluteal muscle and right paralumbar muscles at the level of L4 and L5 were noted. Positron emitted tomography scan confirmed no other metastases. He underwent wide excision of the right paraspinal mass and buttockectomy for the left gluteal mass.
Conclusion: SMM in RCC is rare, thus tissue diagnosis and imaging is deemed necessary to rule out any other primary sarcoma. In these cases, patients may benefit from metastasectomy. Regular follow-up and surveillance are recommended for these patients to rule out recurrence.
Keywords: Renal cell carcinoma, metastases, extraskeletal, buttockectomy.
Reference:
1. Graves A, Hessamodini H, Wong G, Lim WH. Metastatic renal cell carcinoma: Update on epidemiology, genetics, and therapeutic modalities. ImmunoTargets Ther 2013;2:73-90.
2. Sakamoto A, Yoshia T, Matsuura S, Tanaka K, Matsuda S, Oda Y, et al. Metastasis to the gluteus maximus muscle from renal cell carcinoma with special emphasis on MRI features. World J Surg Oncol 2007;5:88.
3. Surov A, Hainz M, Holzhausen HJ, Arnold D, Katzer M, Schmidt J, et al. Skeletal muscle metastases: Primary tumours, prevalence, and radiological features. Eur J Radiol 2010;20:649-58.
4. Sountoulides P, Metaxa L, Cindolo L. Atypical presentations and rare metastatic sites of renal cell carcinoma: A review of case reports. J Med Case Rep 2011;5:429.
5. Ramchandani P. Post-treatment surveillance of renal cancer renal cell. In: Patel U, editor. Carcinoma of the Kidney. 1st ed. Cambridge: Cambridge University Press; 2008. p. 185-202.
6. Goger Y, Piskin M, Balasar M, Kilinc M. Unusual Presentation of Renal Cell Carcinoma: Gluteal Metastasis. Case Reports in Urology; 2013.
7. Haygood TM, Sayyouh M, Wong J, Lin J, Matamoros A, Sandler C, et al. Skeletal muscle metastasis from renal cell carcinoma. Sultan Qaboos Univ Med J 2015;15:327-37.
8. Crispen PL, Blute ML. Role of cytoreductive nephrectomy in the era of targeted therapy for renal cell carcinoma. Curr Urol Rep 2012;13:38-46.
| How to Cite this article: Goyal AK, Vaish A, Vaishya R, Baweja P| A Rare Recurrent Chondromyxoid Fibroma of the Proximal Tibia in an Adolescent Female | Journal of Bone and Soft Tissue Tumors | September-December 2020; 6(3): 20-25. |