Retrospective Study of Seven Patients with Tumoral Calcinosis
Original Article | Volume 6 | Issue 2 | JBST May-August 2020 | Page 12-16 | Kshitij Manerikar, Abhijeet Salunke, Jaymin V. Shah, Mayur Kamani, Shashank Pandya. DOI: 10.13107/jbst.2020.v06i02.25
Author: Kshitij Manerikar[1], Abhijeet Salunke[1], Jaymin V. Shah[1], Mayur Kamani[1], Shashank Pandya[1]
[1]Department of Surgical Oncology, Gujarat Cancer Research and Institute, Ahmedabad, Gujarat, India.
Address of Correspondence
Dr. Kshitij Manerikar,
A-302, Divyadeep, Ram Mandir Road, TPS-3, Borivali West, Mumbai – 400 092, Maharashtra, India.
E-mail: drkshitijmanerikar@gmail.com
Abstract
Introduction: Calcium deposition in the skin has been termed as calcinosis cutis. Tumoral calcinosis is idiopathic form of calcinosis cutis. Etiology of idiopathic calcinosis cutis is unknown. It is characterized by periarticular deposition of amorphous calcium salts around large joints. Our diligent search through literature could not find any consensus on the etiopathogenesis and treatment modalities for tumoral calcinosis.
Materials and Methods: A retrospective study of seven patients of tumoral calcinosis treated with complete surgical excision over a period of 1 year was done. Demographic details were compiled. Routine blood investigations were performed. All patients underwent radiographs and magnetic resonance imaging (MRI) scans of involved part. We did not perform computed tomography (CT) or bone scan in any of our patients. All seven patients underwent surgery and were followed up till 2 years.
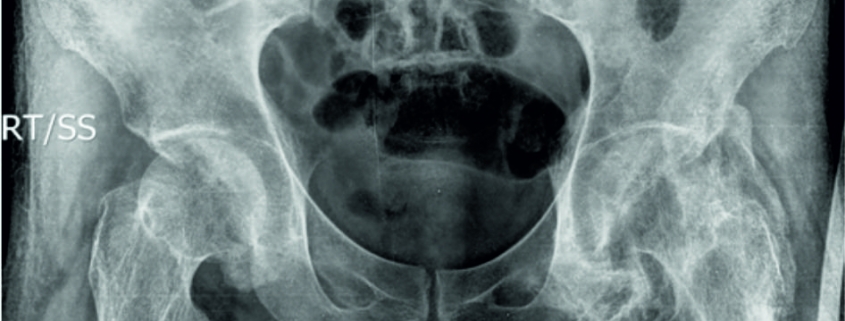
Results: In our study, five were female and two were male patients ranging from 31 to 76 years. Size of swelling varied from 2 to 15 cm. Most common location was hip. Serum calcium, phosphorus, and alkaline phosphatase were normal in all patients. Radiographs showed well-outlined periarticular cluster of calcifications in the soft tissues around joint. MRI revealed round to oval multiple cystic lesions around the affected region, but not involving the joint.
Conclusion: Tumoral calcinosis is always the diagnosis of exclusion. It can be normophosphatemic or hypophosphatemic subtype. Large joints are more commonly affected. One can rely on radiographs for diagnosis. MRI for knowing exact location of lesion, its relationship with adjacent structures and planning of surgery is advocated. Complete surgical excision is the only optimum treatment of tumoral calcinosis.
Keywords: Amorphous calcium phosphate, hyperphosphatemia, X-ray film, hip joint, calcinosis, magnetic resonance imaging.
Reference:
1. Kluger G, Kochs A, Holthausen H. Heterotopic ossification in childhood and adolescence. J Child Neurol 2000;15:406-13.
2. James W, Berger T, Elston D. Andrews’ Diseases of the Skin: Clinical Dermatology. 11th ed. Philadelphia, PA: Elsevier, Saunders; 2011. p. 516-8.
3. Chaabane S, Chelli-Bouaziz M, Jelassi H, Mrad K, Smida M, Ladeb MF. Idiopathic tumoral calcinosis. Acta Orthop Belg 2008;74:837-45.
4. Muddegowda P, Lingegowda J, Ramachandrarao R, Konapur PG. Calcinosis cutis: Report of 4 Cases. J Lab Physicians 2011;3:125-6.
5. Emery K, Fletcher B. The soft tissues. In: Kuhn JP, Slovis TL, editors. Caffey’s Pediatric Diagnostic Imaging. 10th ed. Philadelphia, PA: Mosby; 2004. p. 2009-11.
6. Inclan A, Leon P, Camejo MG. Tumoral calcinosis. JAMA 1943;121:490-95.
7. Smack D, Norton S, Fitzpatrick J. Proposal for a pathogenesis-based classification of tumoral calcinosis. Int J Dermatol 1996;35:265-71.
8. Noyez J, Murphree S, Chen K. Tumoral calcinosis, a clinical report of eleven cases. Acta Orthop Belg 1993;59:49-54.
9. Aprin H, Sinha A. Tumoral calcinosis: Report of a case in a one year old child. Clin Orthop 1984;185:83-6.
10. Niall D, Fogarty E, Dowling F, Moore D. Spontaneous regression of tumoral calcinosis in an infant: A case report. J Pediatr Surg 1998;33:1429-31.
11. Fujii T, Matsui N, Yamamoto T, Yoshiya S, Kurosaka M. Solitary intra-articular tumoral calcinosis of the knee. Arthroscopy 2003;19:E1.
12. Bittmann S, Gunther M, Ulus H. Tumoral calcinosis of the gluteal region in a child: Case report with overview of different soft-tissue calcifications. J Pediatr Surg 2003;38:E4-7.
13. Rodriguez-Peralto J, Lopez-Barea F, Torres A, Rodriguez-Gonzalez JI, Diaz-Faes J. Tumoral calcinosis in two infants. Clin Orthop 1989;242:272-6.
14. Enzinger F, Weiss S. Soft Tissue Tumours. St Loius: C V Mosby; 1983. p. 906-8.
15. Hruska K, Lederer E. Hyperphosphatemia and hypophosphatemia. In: Favus MJ, editor. Primer on the Metabolic Bone Diseases and Disorders of Mineral Metabolism. 4th ed. Philadelphia, PA: Lippincott Williams & Wilkins; 1999. p. 246-53.
16. Salutario M, Vogler J, Harrelson J, Lyles K. Imaging of tumoral calcinosis: New observations. Radiology 1990;174:215-22.
17. Martinez S. Tumoral calcinosis: 12 Years later. Semin Musculoskelet Radiol 2002;6:331-9.
18. Martinez S, Vogler J, Harrelson J, Lyles K. Imaging of tumoral calcinosis: New observations. Radiology 1990;174:215-22.
19. Savaci N, Avunduk M, Tosun Z, Hosnuter M. Hyper-phosphatemic tumoral calcinosis. Plast Reconstr Surg 2000;105:162-5.
20. Yamaguchi T, Sugimoto T, Imai Y, Fukase M, Fujita T, Chihara K. Successful treatment of hyperphosphatemic tumoral calcinosis with long-term acetazolamide. Bone 1995;16:247-50.
21. Slavin R, Wen J, Kumar D, Evans E. Familial tumoral calcinosis. A clinical, histopathologic, and ultrastructural study with an analysis of its calcifying process and pathogenesis. Am J Surg Pathol 1993;17:788-802.
| How to Cite this article: Manerikar K, Salunke A, Shah JV, Kamani M, Pandya S | Retrospective Study of Seven Patients with Tumoral Calcinosis | Journal of Bone and Soft Tissue Tumors | May-August 2020; 6(2): 12-16. |